Do you get irritable sensations in the eye? Do your eyes feel sore, gritty or tired? Do you feel like your eyes are burning, itching or excessively watery? If so, you could be suffering from ‘Dry Eye Syndrome’. Continue reading to understand what Dry Eye is, how your physician will diagnose it and what could be the possible causes.
Dry Eye Syndrome
It is a condition that most customers easily overlook or become dismissive about, but ‘Dry Eye’ syndrome, if not managed, can lead to discomfort, blurry vision, excessive ‘tearing’ and ‘tired eyes’. More often than not, the patients misdiagnose the symptoms and make an assumption that there is something wrong with their spectacles, or that their eyes are tired due to working long hours. Whatever their reasoning, they fail to identify that these symptoms could possibly be from a dry eye condition.
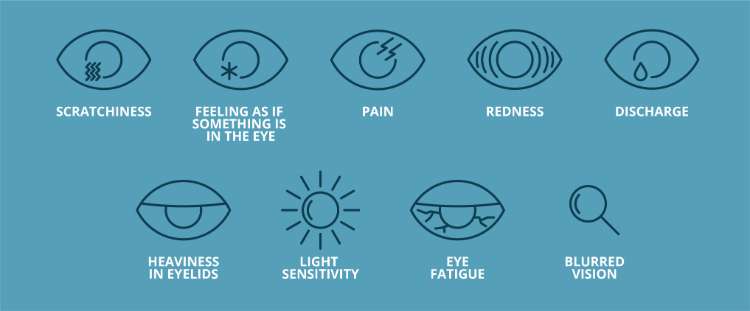
Image (1) Dry eye symptoms: courtesy of Barnet Dulaney Perkins Eye Center
What is Dry Eye?
Dry eye is medically termed as ‘Keratoconjunctivitis Sicca’ and it refers to the disruption of the ‘tear film’. The tear film is a thin layer of clear liquid that sweeps across the eye by the action of every blink.
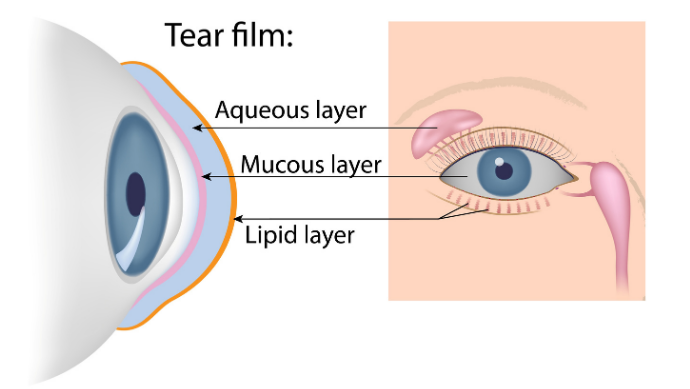
Image (2) Tear Duct: Credit – American Optometric Association
The Tear Film
Tears are produced by various glands surrounding the ocular orbit and its margins. The tear film comprises of three layers. The outermost ‘lipid layer’ is produced by the ‘meibomian glands’, situated at the edge of the eyelids, and its function is to reduce evaporation and lubricate the eyelids. The thickest, middle zone is the ‘aqueous layer’. It is produced by the lacrimal gland which is the almond-shaped gland, positioned in the upper lateral corner of the orbit. This moisturising, watery layer provides corneal nutrition, oxygen supply and flushes away debris. The innermost ‘mucous layer’ forms a continuous moist cover over the eye. It is produced by the conjunctival* cells and masks foreign bodies in the eye to protect the cornea from abrasion.
The eyelids are essential for eye protection and secretion of tear-film products. With each blink, the eyelid ‘washes’ the eye. The tear-film in turn, fills in any surface irregularities over the cornea, to provide a smooth optical surface. If this is disrupted, image-forming light, at the corneal surface, will scatter and is observed as a blurred image. The tear film lubricates the ocular surface keeping the eye comfortable. Some tears will evaporate, some are absorbed by the conjunctival cells and the remaining tears are drained at the extreme nasal edge into the lacrimal puncta and tear ducts.
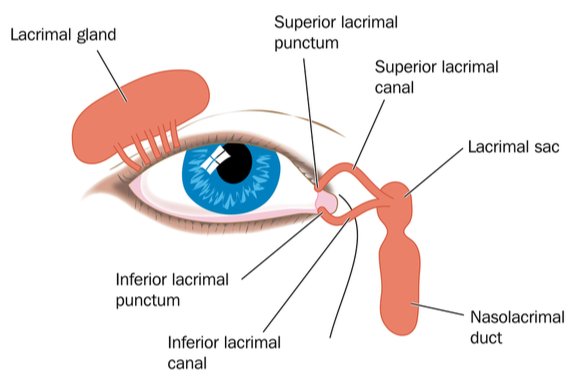
Image (3) Tear Duct: Credit – Lacrimal Duct
Symptoms of Dry Eye
A ‘symptom’ is the condition expressed by the patient. Hence, these are some of the symptoms one would describe in a clinical examination.
- Sore eyes
- Grittiness
- Itchy eye
- Burning sensation
- Watery eyes
- Difficult to open eyes in the morning
- Reduced ‘contact lens’ comfort
- ‘Red’ eye
- Tired eyes
- Blurred vision
- ‘Dandruff’ on eyelashes
- Sticky eyes
- Sensitivity to light (photophobia)
Signs of Dry Eye
A ‘sign’ of any condition is the examination made by an observer or clinician. Opticians will check the tear quality and quantity using various methods. These methods are devised to be as non-invasive as possible to avoid reflex watering. It is a protocol to ask relevant questions to decipher the cause of any underlying issue. A thorough examination of the eyelashes and eyelids will also aid any conclusion to the assessment.
Tear Quality:
To check the ‘quality’ of the tears, a practitioner will observe the ‘tear break up time’ (TBUT) under an advanced microscope, called a slit-lamp. It is a clinical test to measure how quickly the tears evaporate from the surface of the eye. This would entail adding a fluorescein dye to the white of the eye and observing the tears under a cobalt blue light on the slit lamp. The fluorescein will glow brightly under the blue light and before the dye is flushed away by the action of blinking the TBUT is measured. The patient is asked to hold a blink whilst the tear quality is being observed. The optician will measure in seconds how long it takes for a dry spot to appear after a blink (see image 4). More than 10 seconds is a good TBUT and less than 5 seconds would be considered a low TBUT, suggesting a poor tear film1.
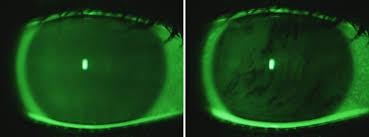
Image (4) Tear film in-tact after a blink, followed by a break in the tear film.
Image Credit: VARPA Group
A non-invasive test of TBUT would be to check the tears under an optical instrument called a Keratometer. This instrument measures the curvature of the cornea but it can also measure the TBUT by observing the images through the instrument. We refer to the Keratometer images as ‘mire’. The clinician will observe the clarity of these mires between each blink. The patient is asked to blink and hold the blink until the mires begin to distort, indicating the evaporation point of the tear film.
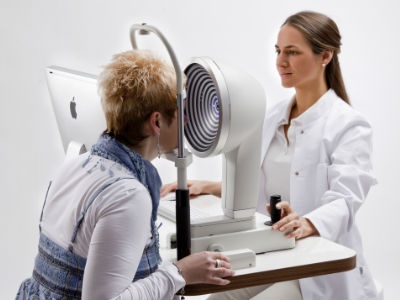
Image (5): Keratograph assessment
Another, non-invasive method of measuring the tear quality, is to use a Keratograph (image 5). This instrument uses a high definition camera to assess the corneal surface and curvature2. It utilises a controlled light source to avoid ‘induced dry eye’ during the test. The instrument is held quite close to the eye, and circular images are viewed by the practitioner using a desktop-software system. Clear circular rings will be observed post blink, and the NIKBUT (non-invasive Keratograph break up time) is measured by when the clear rings begin to distort. The most advanced Keratograph machines will measure tear ‘quality’ as well as the ‘quantity’.
Tear Quantity:
The quantity of tears can be measured in a few ways. Once again, measures are taken to keep these tests as least invasive as possible. The commonly practiced way to measure tear volume is to view the reservoir of tears at the lid margins using high magnification under the slit-lamp. The tear levels, at the lid margins, referred to as ‘tear meniscus height’ (image 6), are graded as minimal, normal or excessive3. Where the slit-lamp is fitted with a measuring device or graticule, the exact height of the tear meniscus can be recorded. The previously mentioned Keratograph will also measure the tear meniscus height.
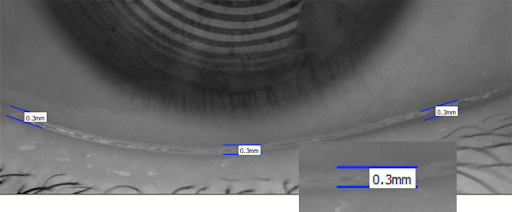
Image (6): Tear meniscus height. Image credit – Society of Ophthalmology Madrid
A slightly more invasive procedure and therefore the less administered test is to apply a very thin, but absorbent strip of paper at the lid margin. After 5 minutes, the amount of the ‘wet’ strip is measured in millimetres. A wetting length of 15mm would be considered normal4. This is referred to as the ‘Schirmer test’.
Other signs of Dry Eyes:
An optician will begin their assessment with the least invasive test first. This will often start with basic observations under diffuse light and then progressively become brighter lighting and greater magnification of the instrument during the test. This allows the optician to view all the relevant layers to be examined.
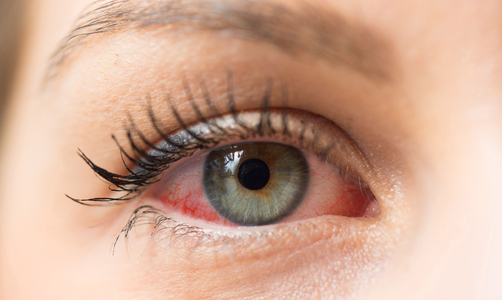
Image (7) Dry Eye
- Visual examination of lid margins may expose irregularity of the glands on the eyelids which can affect the tear film distribution or production.
- Using the slit-lamp under a specific magnification and illumination can highlight debris in the tears, suggesting poor washing of the ocular surface.
- Meibomian glands on the eyelids will be gently pressed to see the expression quality. The fluid should be clear and colourless. Any deviation of this would suggest blocked glands. Severely blocked glands manifest as cysts or styes.
- Visible blood vessels on the white of the eye, known as ‘conjunctival hyperaemia’ would be indicative of dry eye due to exposure or evaporation. See image 7.
- Observing the white of the eye again, are there any signs of discolouration or uneven surface areas? Exposure to wind and UV can give rise to a ‘pinguecula’ (image 8) or ‘pterygium’ (image 9). The former manifests itself as a yellowish, fatty deposit on the outer white of the eye. The latter condition is pink in observation and encroaches the cornea. Both are indicative of dry-eye.
- Eyelashes are checked. Lashes should be clean and growing in the same outward direction. Lashes that grow inwards will irritate the ocular surface. The practitioner will check for Blepharitis which is inflammation of the eyelid. It exhibits itself as a dandruff-like or flaky substance on the lashes. Traces of make-up would suggest poor cleaning of the lashes.
- Is the patient blinking adequately? How much does the px blink and are the blinks partially open? Impartial blinking will lead to dry-eye caused by exposure.
- For contact lens wearers, the lenses may appear more deposited giving rise to discomfort.
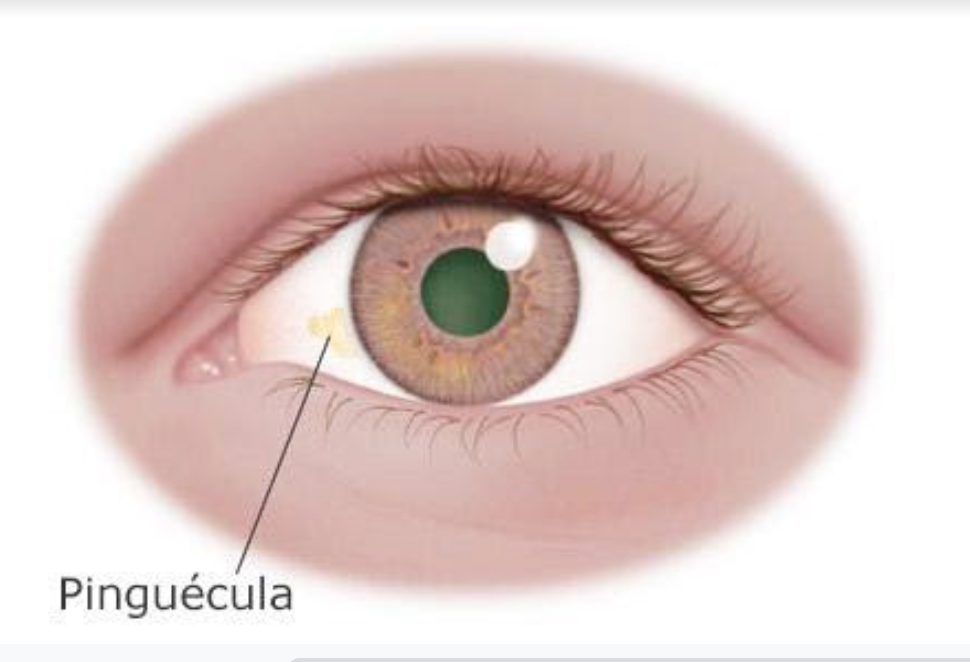
Image (8) Pinguecula. Image credit: cdopv.com – eye conditions
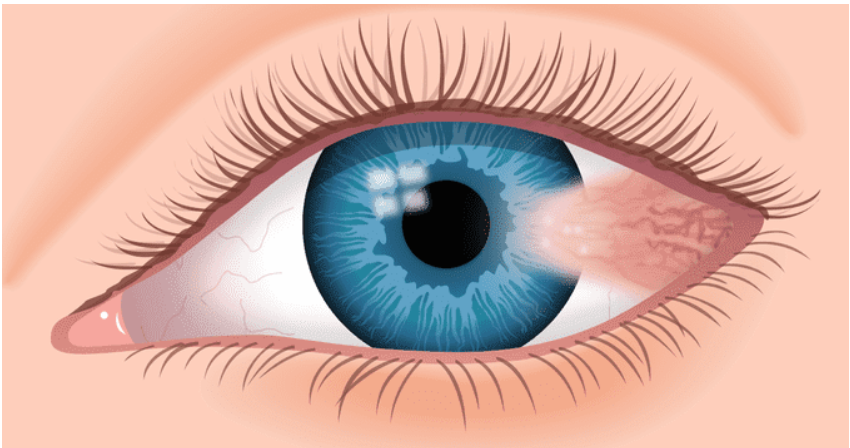
Image (9) Pterygium. Image credit: All About Vision
Factors & Causes of Dry Eye
- Health: Arthritis (reduced fluid secretion), Sjogren’s syndrome (an autoimmune disorder), high blood pressure, digestive problems (vitamin A deficiency)5, thyroid issues, eczema, menopause (hormonal changes produce less fluid), diabetes (lacrimal gland nerves become affected).
- Medicines: Contraceptive pill, anti-histamine tablets, diuretics, tranquillisers, anti-depressants, cancer treatments, hormone replacement therapy (HRT), Beta-blockers.

Image (10) courtesy of Everyday Health
- Allergies: Hay fever (excessive rubbing and itching of eyes), preservatives in eye drops

Image (11): Shutterstock
- Age: Reduction in the quality of tear production as we age
- Gender: Higher prevalence in females6
- History: Recurrent conjunctivitis, eye surgeries (disruption of tear film), ocular trauma
- Work Environment: Air conditioning, VDU use (staring at the VDU monitor), central heating, pollution, if working outdoors there is increased exposure to the elements (extreme cold, wind and UV exposure), dust/debris particles
- Contact Lenses: highly deposited contact lenses (CL), in-correct fitting of CL, type of CL material
- Poor Blinking: Sleeping with eyes partially open, not blinking enough especially when concentrating on tasks
- Eyelid & Eyelash Aetiology: Blepharitis, Meibomian Gland Dysfunction, Ectropion (outward turning eyelid margin) leading to exposure and tear overflow, Entropion (eyelid folds inwards), eye make-up (eyeliner and mascara soil the lid margins)
- Diet: Not drinking enough water (dehydration), alcohol consumption7, diet low in essential Omega oils8, Vitamin A deficiency9


Image (12) Credit: Omega Capsules & Healthy Eyes
- Recreation: Swimming (reaction to pollutants or chlorine), UV exposure, prolonged reading, high altitude activities
- Lifestyle: smoking (the smoke is an irritant, but long-term smoking causes oxidative damage to the tear layers), daily stress10.
READ PART 2 FOR DRY EYE ‘MANAGEMENT SOLUTIONS’
* The conjunctiva is the thin clear membrane that lines the inner eyelids and the front surface of the eye
1. ncbi.nlm.nih.gov – PMID: 23408791
2. Oculus.de – Topography/Keratograph 5M
3. Jnjvisioncare.co.uk – assessment of the tearfilm
4. Jnjvisioncare.co.uk – assessment of the tearfilm
5. ncbi.nlm.nih.gov – PMID: 27708515
6. Rpbusa.org – Gender & Dry Eye
7. Coopervision.com – What is the effect of alcohol on the eye?
8. Healthline.com – Home remedies for dry eye
9. Allaboutvision.com – Eye benefits of vitamin A and beta-carotene
10. Healio.com – use integrative approach to stress-induced dry eye
Posts by Oodo may include affiliate links. This means that we make a small commission from referrals and purchases at no extra cost to you. Thank you for your kind support.








